It started last year (2017), when I was extremely fatigued for months and couldn’t shake the exhaustion. I slept at night as usual, but had a hard time getting up in the morning. The exhaustion, pain and swelling were always present, and no matter what I tried, the discomfort would not subside.
I went to my primary doctor, who sloughed off my symptoms as being tied to inflammation associated with Fibromyalgia. The doctor told me to take calcium and turmeric and sent me on my way. By December, my gums were very inflamed and my tongue was burning. I went to my primary and again was told that it was from the Fibromyalgia. This time, the doctor gave me thyroid medication for a thyroid condition I didn’t have.
Between January and February, my tongue burning came and went and I had canker sores — or so I thought. The canker sores never fully disappeared. I tried to solve the issues using acupuncture, Chinese herbs and vitamin drips. Unfortunately, the natural route was not working. If anything, it was getting worse. Three different doctors misdiagnosed me again — this time with oral thrush — and I spent a lot of time and money on medications I never needed. I went to six different doctors, three of whom said they didn’t have a clue what I had. With no help or guidance, they gave me Prednisone and sent me on my way.
I even had a follow-up with my primary who never showed up to the office. I changed my primary doctor.
Dr. Google
At that point, I was overly frustrated. I started researching “mucous membranes blisters” and luckily information showed about Pemphigus Vulgaris and The International Pemphigus & Pemphigoid Foundation.
““Pemphigus” is used in a very specific way to describe blistering disorders caused by autoantibodies against some part of the epidermis, which lead to disruption of the intercellular junctions (and hence bullae). Pemphigus vulgaris, not surprisingly, is the most common type of pemphigus (“vulgar-” comes from the Latin vulgaris, meaning the general public). It occurs primarily in adults between the ages of 30 and 60, and is characterized by big, flaccid bullae that burst easily (in most patients, you’ll see more ruptured, scab-covered bullae than intact ones). Patients often present first with oral bullae and ulcerations, and later develop bullae on the skin.
In this disease, patients have autoantibodies against desmogleins, which disrupt the connections between the squamous cells of the epidermis and cause very superficial, intraepidermal, fragile bullae. If you do immunofluorescence on the skin, you’ll see a kind of outlining of each individual epidermal cell (because there are autoantibodies bound to the junctions between the cells). Treatment consists of immunosuppressive agents; prognosis is variable, but many patients have a higher than normal mortality rate.” (Dr. Kristine Krafts at the University of Minnesota School of Medicine).
Communication and Trust
Suddenly, I realized Pemphigus Vulgaris was likely the source of my symptoms. If I hadn’t found this information or site, I don’t know where I would be right now, since none of the other specialists knew where to send me or even bothered with helpful suggestions. I brought the information I received from the executive director of the Pemphigus Organization — Mark Yale — to a dermatologist. I wanted to ask for the correct biopsy to be done. The biopsy is a immunofluorescent of the blisters. Before any test results came back, the first dermatologist said she felt I had Behcet’s disease, another rare disease. I underwent all the testing for this disease and saw a rheumatologist, who also felt I had Behcet’s disease. Both doctors did their diagnostic testings and treated me with Prednisone and Colchicine, an immunosuppressant for Behcet’s.
However, when the biopsy results came back, the results were not Behcet’s, but showed positive for Pemphigus Vulgaris. For two weeks, after the results were given, both doctors had me on the wrong immunosuppressant. The dermatologist said she spoke to my rheumatologist to find out she lied and never called him. Two weeks I waited to see the rheumatologist, for him to ask me why wasn’t my medication changed to the correct immunosuppressant for PV. The first medication given is Cellcept. I didn’t have an answer except that my doctors didn’t communicate with one another. My rheumatologist had the results the same day my prior dermatologist had them. He never bothered to look at them until I was sitting in his office.
Angry and confused, luckily I found the International Pemphigus & Pemphigoid Foundation, which directed and guided me. Just coincidentally, the organization was having an in-person group meet up that weekend where I was able to get the name of the Pemphigus Vulgaris expert in the area — a dermatologist who is an expert in this Harry Potter-sounding rare disease. I finally got some answers, and was put on the right treatment plan.
“Pemphigus is estimated to affect anywhere from 0.7–5 people per 1,000,000 per year in the general population.”
How did this happen? Why me?
Organic diet, exerciser, healthy individual who never took antibiotics to having a never heard of rare disease can take a toll not only on your body but your mind.
Relationships where you were the strong one, the go-to one for help has now changed to unless you could listen and give advice, you no longer have communication with those individuals. When they ask how you are doing and you tell them not great, they don’t hear you and just jump to their problems for you to solve. Thanks to the disease plus medications, my focus many times, was not there so I didn’t respond or give much back to the conversation, so the conversations would end quickly; never to hear from them again.
Social Media Not So Social
Most of my career has been online marketing and having to promote brands and products. However, for my own social media, I rarely post about anything personal. Due to this rare disease called Pemphigus Vulgaris plus being misdiagnosed with Behcet’s, another rare disease, I felt a need to bring awareness to others. So, I decided to share a bit on social media. The individuals who I thought were closer to me didn’t respond or told me they would keep me in their thoughts.
Information Overload
Fortunately, we have the internet, so it’s easy to do a Google search and see right away what this crazy disease is. I had Celiac Disease when it was relatively unknown. It wasn’t as easily diagnosed as it is today. Still, 17 years ago, we changed my diet to keeping gluten out of it. Back then I got similar responses, telling me it was in my head and how food couldn’t make me bedridden. When my husband found me on the floor and I couldn’t get up due to my nerves not responding, it was clear it wasn’t in my head.
The individual going through the disease has a lot to deal with and I get it that most people do not know how to respond to some weird named, not contagious, autoimmune disease unless you say it’s Cancer.
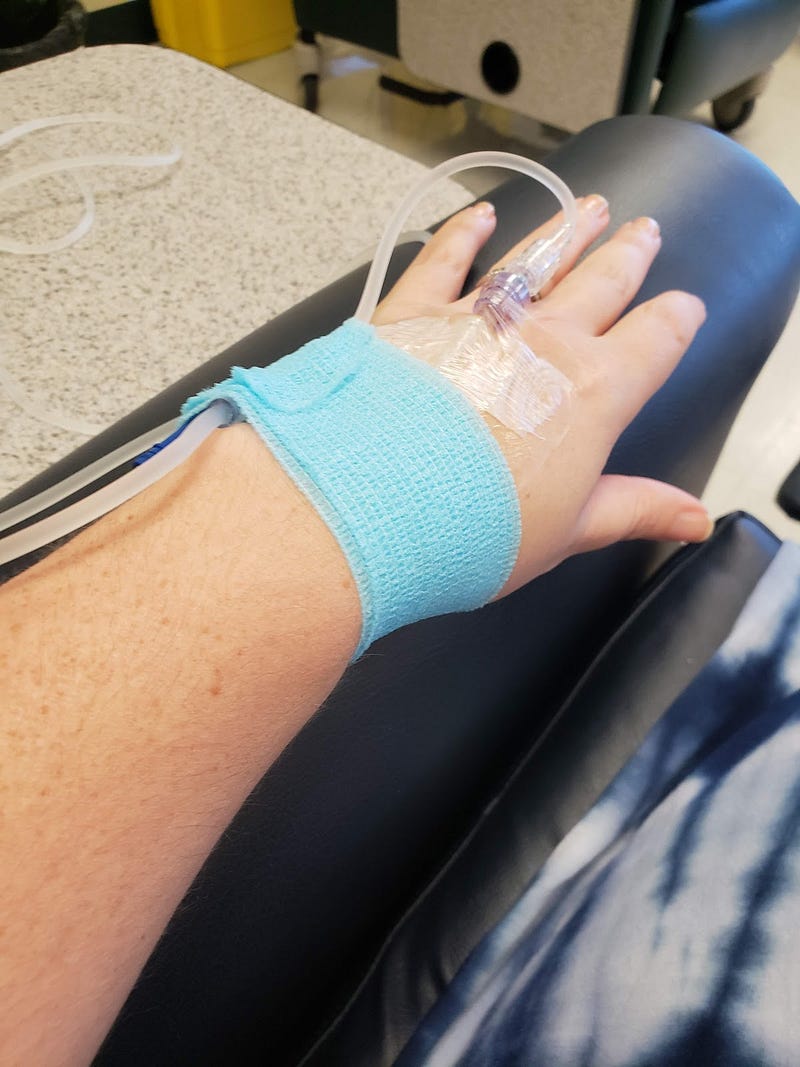
Guess what, the Rituxan treatment they pumped into my vein for six hours is a lymphoma treatment. It involves chemicals — which I have worked so hard to keep out of my body for 42 years — being shot directly into my blood to kill off my B cells and immune system so the blistering of my mucous membranes, scalp and skin will eventually stop. But Rituxan takes weeks of waiting to see if it will calm the disease down.
According to my doctor, Dr. Angela Weatherall of ClearlyDerm, “Rituxan peaks at 11 weeks so every two weeks as the prednisone is lowered, the Rituxan treatment should improve the PV’s condition.” But like many other diseases, each case is dependent on the individual. Some PV sufferers have had four Rituxan infusions and not gone into remission while others after the first round have. Unfortunately, it is a lot of taking the medications and waiting for the outcome.
What is Rituxan (rituximab)?
Rituxan (rituximab) is a B-cell antibody treatment option for patients with pemphigus that is being used as first line therapy by many clinicians.
How does it work? B-cells are responsible for producing antibodies for the body, rituximab works as an immunosuppressant that destroys B-cells of the immune system. A course of rituximab is administered with the hope that it will destroy all the B-cells that make antibodies in pemphigus or pemphigoid are removed. Retreatment with rituxan may be required, usually at six months or longer after the initial treatment.
FDA Approval
In June of 2018, the U.S. Food and Drug Administration (FDA) approved Rituxan® (rituximab) for the treatment of adults with moderate to severe pemphigus vulgaris (PV). Earlier in the year, the FDA had granted Priority Review, Breakthrough Therapy Designation, and Orphan Drug Designation to Rituxan for the treatment of PV.Rituxan is the first biologic therapy approved by the FDA for PV and the first major advancement in the treatment of the disease in more than 60 years.
Source: https://www.rituxanforpv.com/
The blisters are not normal blisters, they open easily and then cause other infections. Imagine having burns that don’t heal. I had blisters in my throat, larynx, tonsils, gums, face, nose, scalp, tongue, lips and thighs for months, and still have a few. I have a scar in my throat where I had a bunch of blisters. At the worst, the pain and swelling was so insane that I stopped breathing one night.
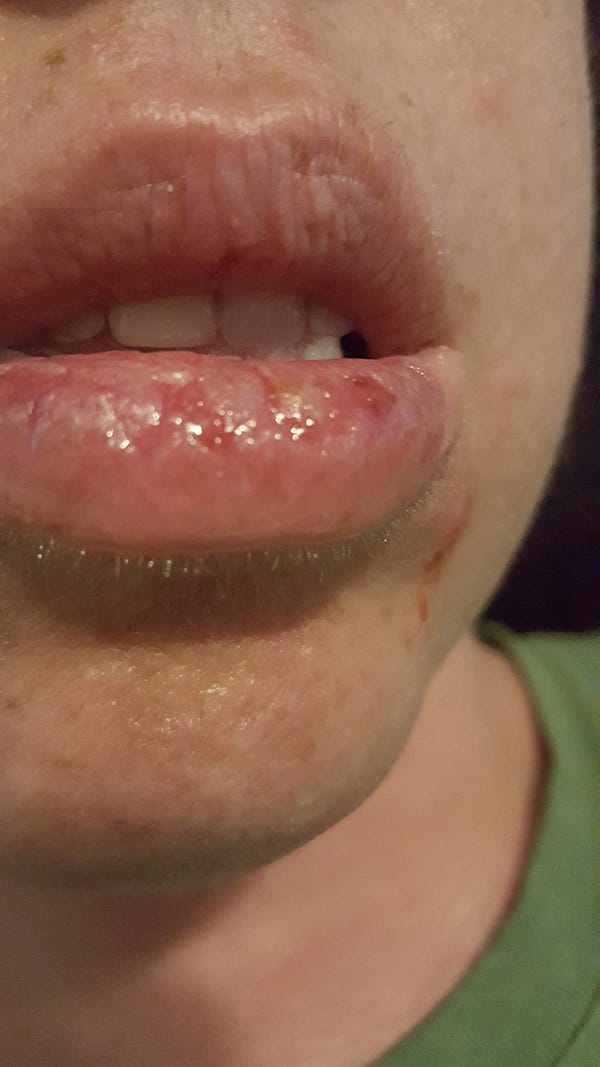
What I have found going through this autoimmune disease — and still going through it, as I completed my first round of Rituxan infusion treatments in August — is that a lot of people ask about the condition, but they don’t listen. And if someone really wants to know about what the disease is or how you are truly doing, they will shut up, listen and engage. Why do I know this? Because I am fortunate to have a small group of friends, and family, who check in with me a few days a week just to make sure I am OK.
No one asks to be given a chronic rare disease. There are days you feel like yourself and take advantage of those good feelings, because you never know what the next day will bring. That’s the problem: There are days where all you can do is sleep, and other days where you feel you can run a marathon. As others dealing with autoimmune diseases know, if your body hasn’t run a marathon in a while, don’t do it (unless you have been training) but take advantage and get out of the house and enjoy life.
There are days where your mind and brain fog is so bad you don’t know if it’s from the disease or the medications.
Being on prednisone is horrible! Tapering down I get excited and hope I can be off it without new blisters appearing. Odd things occur from muscle spasms, swelling, hormone imbalance, high blood pressure, hypoglycemia, hair loss, quick weight gain and damage to organs.
Every day, I make sure to do some form of movement, whether it’s stretching, yoga, aerobics or lifting weights. Sometimes, it helps clear my mind, even for an hour, when you feel the fog lift. If you can afford it or your health insurance covers it, acupuncture also helps with overall well-being.
No More Stress
This disease has brought a thought to the forefront of my mind: What do I truly want to do for the rest of my life? I went to college to be an educator and my career path steered into marketing. I’ve had some great experiences and opportunities because of my marketing career. But the truth is I love being an educator and teaching others. Whether it’s through corporate training, online teaching, in-classroom teaching or mentorship, my career and natural talent is to be a teacher.
It’s challenging to have a rare incurable disease and to have to wait three months to see if the infusion treatments will put me into remission. However, the positive side is that being diagnosed with a disease like this makes you take a review of your life. I was able to question whether I am spending the time working in a field that I really want to be in, or if I’m doing it simply because I have to. In the past few months, I have been able to get back into working as a writer in higher education — not only as an English professor, but also a subject-matter expert and curriculum consultant. I have been writing again about topics that I know will help others, and have been taking time for myself to allow my body to heal.
There is still a long road ahead. I am still in treatment and there is a lot of waiting and seeing what the disease will do, as I try to reduce — and eventually eliminate — my intake of daily medications. Rituxan infusions take 11 weeks to know if they will put the disease into remission. If they don’t, then six months from the first treatment — which is February — I can receive another infusion in hopes that it will put the disease into remission.
Support
There are a few private support groups online on Facebook and through Rare Connect. As rare as this disease is, there are other people from all around the world being diagnosed every week! Searching the hashtags #healourskin #raredisease in social media can also connect you with others.
Being able to support each other and share the information allows for exchanges and learnings. For example, while in the midst of the flare, I had easily 60 open blisters within my mucous membranes and lost 35 pounds due to not eating. Even trying to drink water hurt, so I was dehydrated. I couldn’t speak for two months.
From my own experimenting, I found drinking anything creamy — in my case, almond milk or a non-dairy protein shake — was all I could do. The doctors were adamant about me drinking, or they were going to stick me in the hospital for dehydration. I HATE hospitals, so I avoided that. But I wish I found the support groups sooner so I could ask questions. Overnight, the blisters multiplied and the pain was excruciating. Even on steroids, it takes weeks, if not months, for the medicines to start taking effect. Once the pain lessened a little, then my diet consisted of sweet potatoes, cucumbers and fish.

Thanks to prednisone, the weight came back.
Takeaways:
- Living in the Sunshine State and loving the sun, the UV rays can set off the disease. Once it goes into remission, it seems like other PV individuals can go into the sun without a flare. But during a flare, staying out of the sun is advised. Wear sunscreen, hats and UV-protectant clothing.
- Always document through pictures. With cell phones, it has become much easier to keep photos and videos and the dates. Doctors will ask to see proof, especially if you end up on Prednisone by the time you get to the expert.
- Trust yourself, you know your body. For 20 years I’ve had itchiness on my scalp and was told it was allergies, but this may have been PV all along. Itchiness is putting it mildly, I would get what I thought were pimples, but obviously were ulcers. The past few years were bad, and I would use tea tree oil, which calmed my breakouts and healed my scalp from the open wounds.
- Find a dentist who understands Pemphigus and autoimmune diseases. I was given a referral for a dentist and when I went for the consultation, I asked him has he ever had a patient with Pemphigus. He said no, and that I was the second person who he has seen up close with it. He was ready to drill my teeth, which is a big no-no. Dental work will cause a flare, so it’s imperative that you find the right dentist when dental care is needed.
- Having Celiac Disease, diet and vitamins were always part of my life. There is mixed research, some of which says the right diet and taking vitamins will not help fight Pemphigus. But either way, I continue to follow the Celiac protocol. Immune boosting vitamins and supplements are not advised as the immune system is attacking itself and that’s the reason for the immunosuppressant. Why anger the body even more, right?
- Acupuncture has been helpful with the side effects of the medications. Also, it helps ease the mind as many PV sufferers have anxiety and fear that we will wake up one day and the blisters return.
Without treatment, the disease will not go away on its own. As much as I tried natural cures, it continued to get worse. If you don’t get PV under control, the next flare is worse, according to Dr. Weatherall. My first flare was bad, but I know it could have gotten worse if I didn’t get it under control. From diagnosis to Rituxan treatment was less than three months, because I was advocating and being a pain in the ass to get the treatment started.
Patient Advocacy
For anyone going through a rare disease, be your own advocate or have someone who can do it for you! Research and get the information, and share it with your doctors. My oncologist said Rituxan infusions weren’t covered by insurance. I said go check the website — as of June 2018, the FDA has approved the treatment. Minutes later, he came back with the information and apologized. Plus, the company that makes the medication, Genentech, also has a discount program for anything the insurance doesn’t cover. We have to be our own advocate and make our voice heard!
For more information about Pemphigus, visit Pemphigus.org.

Additional Resources:
Video by two doctors: http://phc87.paradigmmc.com/pv_challenges-solutions/toc.php?fbclid=IwAR1HP8ca9FQXGNGfeMLOh55JF8l-uir14CUA_h8Iz68j8xxLzlY6bZFsTLU
Video: Can we cure autoimmune disease? https://www.youtube.com/watch?v=8Oq90aXUd1o

